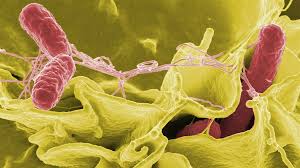
Bacillus cereus is a ubiquitous spore-forming, potential foodborne pathogen that may cause two types of gastrointestinal illnesses: diarrhea and emesis.
 The emetic syndrome results from the presence of a heat-resistant toxin, called cereulide, produced by B. cereus in food products. Although both syndromes are usually mild, with patients recovering after about 24 h, an intoxication can be fatal for vulnerable individuals such as children or elderly people
The emetic syndrome results from the presence of a heat-resistant toxin, called cereulide, produced by B. cereus in food products. Although both syndromes are usually mild, with patients recovering after about 24 h, an intoxication can be fatal for vulnerable individuals such as children or elderly people
In Belgium, from 2007 until 2012, two to eight foodborne outbreaks were reported on a yearly basis in which B. cereus was identified as the causative agent. During this period 8 of 26 B. cereus outbreaks were caused by emetic B. cereus representing 147 cases and 1 death.
In this report, we describe a foodborne outbreak affecting 20 toddlers aged between 10 and 18 months caused by the consumption of a homemade mashed rice–cucumber–chicory meal contaminated with critical levels of the B. cereus emetic toxin.
This outbreak highlights the importance of respecting good hygienic practices and strict storage conditions. An ill staff member had been involved in the preparation of the implicated food and may have contaminated the food. Unfortunately, no fecal sample from the staff member could be analyzed and thus her role could not be confirmed. It is recommended to withdraw any ill person from food preparation activities, as stated by the Codex Alimentarius.
Moreover, the temperature in the refrigerator where the food was stored had never been registered by the director of the kindergarten. The refrigerator at the kindergarten did not meet the Belgian recommendation on refrigeration temperatures, which are recommended to be between 0 and 4_ C, although it was in accordance ( < 7_ C) with the Belgian and European Legislation. Storage of foods below 10_ C prevents the growth of strains that produce emetic toxin, while refrigeration below 4_ C is necessary to prevent growth of all types of B. cereus , including psychrotrophic strains. In this case, high levels of B. cereus were present and cereulide was detected in the leftovers. It is known that cooked rice supports cereulide production at temperatures from 15_ C to 37_ C.
 Therefore, inappropriate and slow cooling probably allowed the development of B. cereus and subsequent cereulide production in the rice. After cooking, the temperature of the food should be allowed to drop to 10_ C as quickly as possible and should ideally reach 4_ C to avoid any growth of B. cereus.
Therefore, inappropriate and slow cooling probably allowed the development of B. cereus and subsequent cereulide production in the rice. After cooking, the temperature of the food should be allowed to drop to 10_ C as quickly as possible and should ideally reach 4_ C to avoid any growth of B. cereus.
Portioning the rice for storage would also have helped to achieve a more rapid drop in temperature below 10_ C in the center of the bowl in which the rice was stored.
Subsequent to this outbreak, a plan for cleaning was established at the kindergarten, and measures for temperature control of the refrigerators were taken.
Given that hazardous levels of cereulide can be reached quickly as demonstrated in this investigation, it is important to remain vigilant during food preparation and food storage to prevent illness and outbreaks caused by B. cereus .
An emetic Bacillus cereus outbreak in a kindergarten: detection and quantification of critical levels of cereulide toxin
Foodborne Pathogens and Disease. January 2015, 12(1): 84-87
Delbrassinne Laurence, Botteldoorn Nadine, Andjelkovic Mirjana, Dierick Katelijne, and Denayer Sarah
http://online.liebertpub.com/doi/abs/10.1089/fpd.2014.1788#utm_source=ETOC&utm_medium=email&utm_campaign=fpd
 EN 24 News reports on Friday Sept. 6 and the following days, 200 pupils and teachers fell ill at the Spermalie hotel and tourism school in Bruges. Laboratory testing of stool languages soon showed that Spermalie was affected by an outbreak of salmonella. The samples of the meals that were served in the school restaurant were then analyzed. An online survey of students and teachers was also launched to find out who had eaten what in which restaurant.
EN 24 News reports on Friday Sept. 6 and the following days, 200 pupils and teachers fell ill at the Spermalie hotel and tourism school in Bruges. Laboratory testing of stool languages soon showed that Spermalie was affected by an outbreak of salmonella. The samples of the meals that were served in the school restaurant were then analyzed. An online survey of students and teachers was also launched to find out who had eaten what in which restaurant.