In Aug. 2008, 26-year-old Chad Ingle had a meal at the Country Cottage in Locust Grove, Oklahoma, a popular family-owned buffet-style restaurant.
Nine days later, Chad was dead from E. coli O111.
By the end of the outbreak, 341 people had been sickened with E. coli O111, all from eating at the country diner in a town of 1,423 people.
Early in the outbreak investigation, health types said it was unlikely that any well water .jpg) contamination was the source of the outbreak.
contamination was the source of the outbreak.
A paper describing the investigation was published last week in
Epidemiology and Infection and concluded from epidemiological evidence the outbreak resulted from cross-contamination of restaurant food from food preparation equipment or surfaces, or from an unidentified infected food handler.
From the paper:
The establishment was out of compliance with five regulations associated with hot and cold holding of foods, food storage, labeling and storage of toxic items, and cleanliness of food contact surfaces. The restaurant did not have written protocols or schedules for cleaning the kitchen, buffet, dining, or bathroom areas. A diluted bleach solution was used to clean surfaces and food spills, but there was no established method for monitoring the concentration.
The restaurant owners disclosed that their private well had been accessed briefly on 10 August to supply water to the restaurant when a sudden interruption of the municipal water system occurred during a lunch period of high volume patronage. The private well was the sole water source for a few hours on this date, but was not accessed again once the municipal water service was restored. The well was physically located
on the restaurant property, which is positioned on a major road on the outskirts of a small rural community.
Pasture land with livestock adjoins the property on the rear aspect of the restaurant. Well water samples collected on 27 and 29 August were positive for total and fecal coliforms. Numerous types of bacteria, including Proteus , Klebsiella , Serratia,
Enterobacter, Pseudomonas , and Pantoea species were cultured from the well-water samples. E. coli isolates were also identified, but none were Stx-producing or serogrouped as O111. PCR testing by the CDC Waterborne Diseases Laboratory also failed to detect the presence of E . coli O111.
To our knowledge this is the largest community outbreak of E. coli O111 on record. Several potential vehicles of introduction and contributing factors for spread within the restaurant were explored, including a primary contaminated food item, an infected food handler, contaminated well water, and cross-contamination from restaurant surfaces or equipment harboring the organism. Multiple specimens representing these potential vehicles were obtained for laboratory testing, but E. coli O111 was not isolated by culture or identified by molecular methods in any of them. The epidemiological findings suggest that foodborne transmission of E. coli O111 through
various food items – either contaminated directly by an infected food handler’s hands or by cross-contamination from food preparation equipment, counter surfaces, or storage areas – occurred at the restaurant.
While bacterial culture and Shiga toxin testing of submitted stool specimens did not identify an infected food handler, epidemiological findings are most consistent with foodborne transmission by an ill employee who continued to work, or by an asymptomatic food handler. Two employees, one with hostess duties and the other a food handler, reported working with diarrheal illness during 15–17 August.
The U.S. Centers for Disease Control says there had been 10 previous outbreaks of E. coli O111, of which four were linked to food. Before the Oklahoma outbreak the biggest O111 .jpg) outbreak happened in New York in 2004. Unpasteurized apple cider was blamed for 212 illnesses.
outbreak happened in New York in 2004. Unpasteurized apple cider was blamed for 212 illnesses.
In 1995, E. coli O111 sickened 173 people and killed a four-year-old girl in Australia, after eating contaminated mettwurst, an uncooked, semi-dry fermented sausage.
A table of non-O157 shiga-toxin producing outbreaks is available at http://bites.ksu.edu/nonO157outbreaks.
Abstract below.
Epidemiology of a large restaurant-associated outbreak of Shiga toxin-producing Escherichia coli O111:NM***
25.nov.11
Epidemiology and Infection, pp 1-11
K.K. Bradley, J.M. Williams, L.J. Burnsed, M.B. Lytle, M.D. McDermott, R.K. Mody, A. Bhattarai, S. Mallonee, E.W. Piercefield, C.K. McDonald-Hamm and L.K. Smithee
http://journals.cambridge.org/action/displayAbstract?fromPage=online&aid=8442046
SUMMARY
In August 2008, a large outbreak of Shiga toxin-producing Escherichia coli (STEC) O111:NM infections associated with a buffet-style restaurant in rural Oklahoma was identified. A case-control study of restaurant patrons and a retrospective cohort study of catered event attendees were conducted coupled with an environmental investigation to determine the outbreak’s source and mode of transmission. Of 1823 persons interviewed, 341 (18·7%) met the outbreak case definition; 70 (20·5%) were hospitalized, 25 (7·3%) developed haemolytic uraemic syndrome, and one died. Multiple food items were significantly associated with illness by both bivariate and multivariate analyses, but none stood out as a predominant transmission vehicle. All water, food, and restaurant surface swabs, and stool cultures from nine ill employees were negative for the presence of Shiga toxin and E. coli O111:NM although epidemiological evidence suggested the outbreak resulted from cross-contamination of restaurant food from food preparation equipment or surfaces, or from an unidentified infected food handler.

.jpg) contamination was the source of the outbreak.
contamination was the source of the outbreak.
.jpg) adding that the effect the outbreak of the illness has on the crop markets is adverse.
adding that the effect the outbreak of the illness has on the crop markets is adverse. farmers markets, groceries, etc., is done to improve food safety.
farmers markets, groceries, etc., is done to improve food safety.  told that without a kidney transplant he would die.
told that without a kidney transplant he would die..jpg) reported Sept. 13. The Health Department has teams in Mustang trying to determine the cause of the outbreak. No children have been hospitalized.
reported Sept. 13. The Health Department has teams in Mustang trying to determine the cause of the outbreak. No children have been hospitalized. Amy spent 6 years doing her PhD at the University of Michigan so figures she’s a Detroit Red Wings fan. Last year, she watched more of the Detroit- Pittsburgh final than I did while we were in Quebec. Detroit just eliminated Chicago in overtime, and I’m still crushed that Carolina lost in 4 games.
Amy spent 6 years doing her PhD at the University of Michigan so figures she’s a Detroit Red Wings fan. Last year, she watched more of the Detroit- Pittsburgh final than I did while we were in Quebec. Detroit just eliminated Chicago in overtime, and I’m still crushed that Carolina lost in 4 games. Locust Grove, Oklahoma, was also hammered by an E. coli outbreak, E. coli O111, linked to dining at the Country Cottage restaurant in August.. One person died, 72 were hospitalized and 241 others got sick before the outbreak was contained.
Locust Grove, Oklahoma, was also hammered by an E. coli outbreak, E. coli O111, linked to dining at the Country Cottage restaurant in August.. One person died, 72 were hospitalized and 241 others got sick before the outbreak was contained.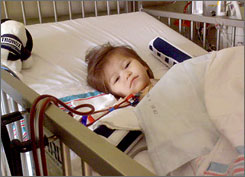 Braylee’s father, Jake Beaver, said after her 12-day hospital stay (family hoto from
Braylee’s father, Jake Beaver, said after her 12-day hospital stay (family hoto from